Liver Transplant Lifeline in Advanced Liver Disease
Liver Transplant Offers Lifeline in Advanced Liver Disease
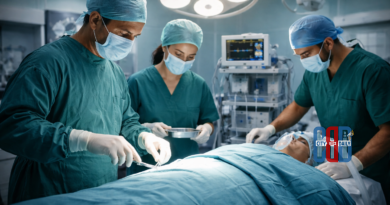
Liver transplant has emerged as a critical life-saving option for patients with advanced liver disease, especially when the organ loses its ability to regenerate and function effectively.
Doctors explain that the liver is the only organ, after the skin, capable of significant regeneration. Even if nearly 70 per cent of it is damaged, the remaining portion can continue performing vital functions. However, when damage progresses unchecked, a liver transplant becomes the only viable treatment.
Causes and Early Warning Signs of Liver Disease
Chronic alcohol consumption, hepatitis B and C infections, fatty liver disease, and obesity are among the leading causes of liver disease. In children, congenital conditions such as Wilson’s disease, absence of bile ducts, and certain metabolic disorders are significant contributors.
In many cases, liver damage develops silently over 10 to 20 years. Symptoms such as yellowing of the eyes, persistent itching, fatigue, loss of appetite, abdominal discomfort, poor concentration, and memory decline appear only in advanced stages. By then, scarring or cirrhosis may have extensively affected liver function.
Health experts advise early screening through blood tests and FibroScan to detect complications before they progress. In the early Child-Pugh ‘A’ and ‘B’ stages, lifestyle modification and medication can help restore function. However, in advanced ‘C’ stage cases, a liver transplant is often necessary.
Liver Transplant: Procedure and Eligibility
A liver transplant involves removing the damaged liver and replacing it with a healthy one from a donor. Donors can be either deceased (cadaveric donation) or living relatives with matching blood groups.
In living donor cases, about 25 percent of the donor’s liver is transplanted. Due to the liver’s regenerative capacity, both donor and recipient livers grow back to near-normal size within weeks. Doctors report success rates of up to 95 percent in suitable cases.
Individuals with active infections, substance abuse issues, or serious heart and lung conditions are not eligible to donate. Healthy blood-related relatives under 50 years are typically considered for donation after a medical evaluation.
Where family donors are unavailable, patients must register under the state-run organ donation program and await allocation from a brain-dead donor. Once a liver becomes available, surgery may take between four and fourteen hours, involving specialized surgical teams.
Post-surgery, patients require immunosuppressive medication to prevent organ rejection and must follow strict medical supervision. With proper care, most recipients can return to normal life after recovery.